
A
meta
-
analysis
on
uterine
transplantation
: R
edefining
the
limits
of
reproductive
surgery
R
ev
A
ssoc
M
ed
B
ras
2016; 62(5):474-477
475
table, where it is initially flushed with heparinized saline
solution, followed by cold preservation solution. The uter-
us is kept on ice until the time of transplantation.
4
Likewise, the receiver’s surgery begins with a subum-
bilical midline incision. First, the vaginal walls are sepa-
rated from the bladder and rectum, and sutures are at-
tached to the round ligament, uterosacral ligament,
uterine rudiment (patients with Müllerian anomaly), or
paravaginal connective tissue (patients with cervical can-
cer) for later transplant fixation. The external iliac vessels
are then dissected bilaterally. The uterus is brought into
the room, still on ice, and placed in the receiver’s pelvis
in an anatomical position. End-to-side vascular anasto-
moses are performed between the vessels of the graft and
the external iliac vessels, after which the clamping of the
external iliac vein is released. A mannitol intravenous bo-
lus is administered immediately before the arterial clamp-
ing is released, and the systolic blood pressure is moni-
tored and maintained above 100 mmHg. After completion
of all vascular anastomoses, blood flow in uterine vessels
is quantified using a Doppler probe placed around the
uterine arteries.
4
The receiver’s vaginal walls are opened using a longi-
tudinal 40 mm incision, and the vaginal portion of the
graft is anastomosed to the Douglas’
cul-de-sac
. The uter-
us is fixed in anatomical position by binding of the su-
tures pre-positioned to their respective ligaments, and by
superimposing the graft’s peritoneum on the recipient’s
bladder.
4
The receiver’s anesthesia and surgery are, in general,
identical to the donor’s. The pre-transplant evaluation of
patients has been extensively described for solid organ
transplantation. The standard protocol published in im-
munosuppression literature consists of a triple regimen
of tacrolimus, azathioprine and corticosteroids, which ap-
pears to be safe during pregnancy. The cases of mild rejec-
tion were successfully treated with pulse steroid therapy.
4
R
esults
Worldwide, 11 uterine transplantations were performed
in patients (Figure 1). In 2000, the first case of uterine
transplant was performed in Saudi Arabia in a 26 year-
-old patient with a history of hysterectomy due to post-
partum hemorrhage, who received the organ from a liv-
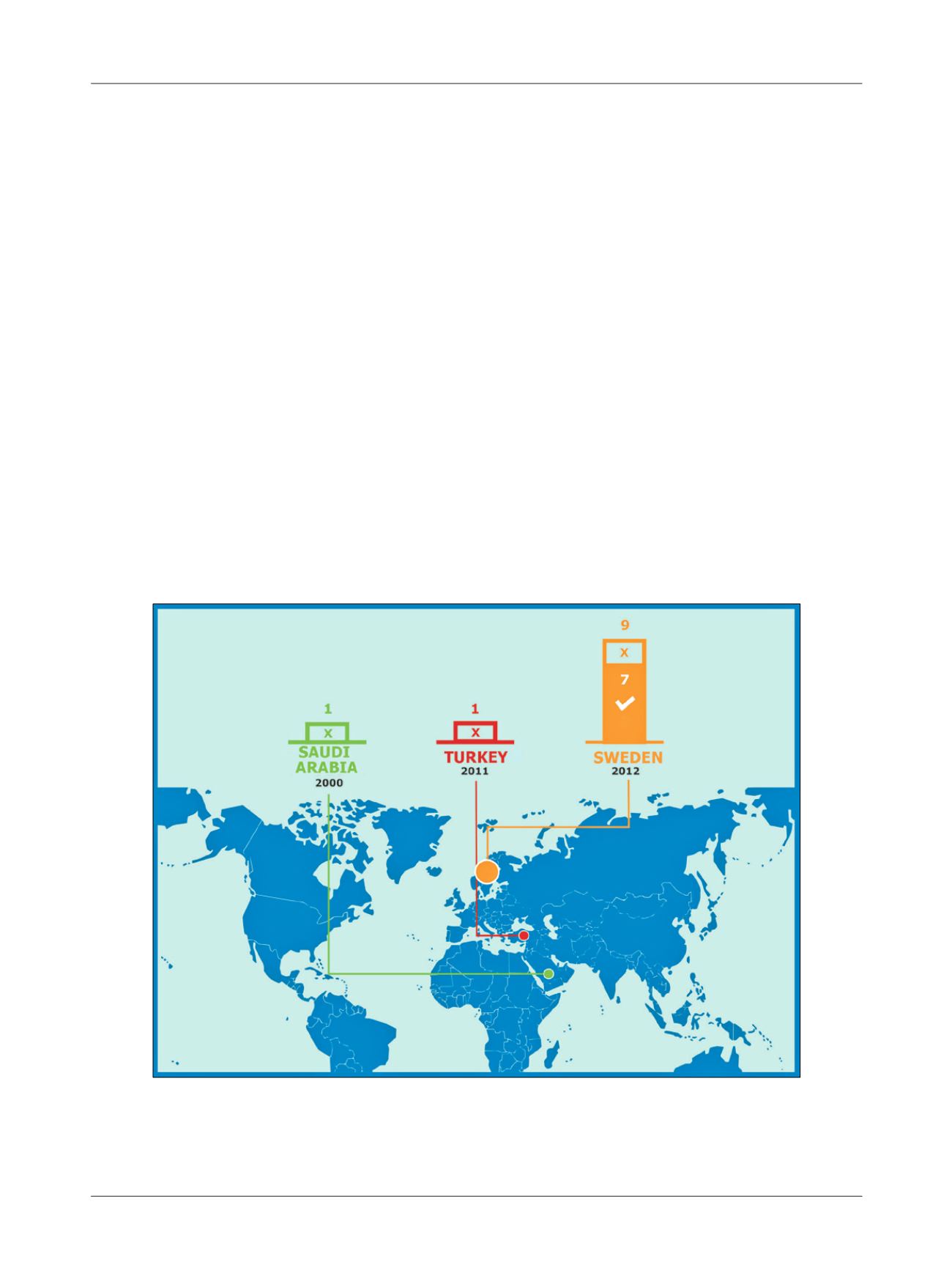
FIGURE 1
On the map, the three centers performing uterus transplantation in humans in the world: Saudi Arabia (N=1) in 2000, Turkey
(N=1) in 2011, and Sweden (N=9) since 2012.
X: Transplant with complications leading to hysterectomy;
: Transplants that maintain reproductive potential.















